|
The tips I learned from one session with the sports psychologist seemed to really help this week! I continue to use the "awareness/be present" tips - accepting the pain, acknowledging there is pain today, and it's just pain for this moment - doesn't mean it's going to be pain forever. This is supposed to help curb that worrying about the future thoughts. When we worry about the unknown, it can case more anxiety and things can hurt more because of the cortisol pumping through your body. I felt like the worrying was under better control this week, but pain still the same or worse (because I walked in the snow and had a steroid shot).
Six days since the steroid shot in the knee. I don't feel any better. If anything I've had some random achy-ness. I was driving today and the knee sent me into Lamaze type breathing because the pain was so sudden, but not like a stabbing pain. Weird! It probably is related to the steroid shot. I am still waiting to hear back from the tendon expert on the other side of the world and for her to answer my questions on the rehab she proposed to me. Still waiting for the Leukotape to arrive as well, so this avenue is on hold until I get more info. Until then, I am resuming my current rehab with emphasis on DOUBLE LEG moves right now:
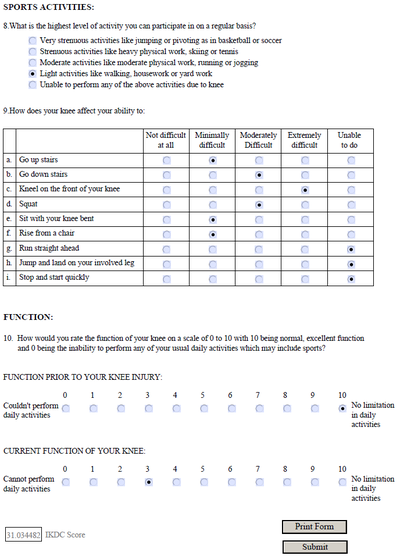
Also, I try to do 30 min of walking (treadmill or outside), some light spinning on a bike, and maybe some gym stuff like the leg press. I dropped the leg press machine down to 10 pounds total, double leg. Yes, I was doing 100 pounds with one leg back in May. I'm going to avoid walking in the snow right now for another month or two. That really hurt too much and set me back on the couch 5 days, plus the pain was still there at night (usually I don't hurt if I lie down). KNEE SCORE UPDATE: About 2 months ago I took some knee score tests: Lysholm and IKDC. Two months later, my Lysholm Knee Score was 32 and now is 34! It seems I couldn't really do any squatting 2 months ago, but now I can manage some mini squats (it's not a full 90 degree squat). I can also go up stairs two at a time (if I concentrate), but the test says one stair at a time or go up stairs normally - which I am in between. IKDC did improve from a 24 to a 31! Going up stairs is getting a little better, it seems overall daily pain went down 8 to a 6? The pain fluctuates depending on what I've done, but it's always a baseline 5.
0 Comments
Yesterday I had a 10+ month post op visit with my physician assistant. Overall I updated him on the "experiment." He reiterated that ACL knees are never going to be normal again, the best case doctors can hope for is 90%. My new "staying in the present" attitude is not going to try to guess when that will be or how much normal I will return to. Just experience and appreciate everyday as it comes.
I was still having a lot of pain perhaps from the Sunday walk in the snow, so much that he could tell by looking at me sitting in the chair trying to find a comfy position. He highly recommended I try a steroid shot in the knee (depo-medrol). I was reluctant at first (OMG I don't have time to research this???). It did not hurt as much as I thought even though the needle goes into the joint cavity! It should kick in by day 3 to 7, if it's going to work. Wow, to be pain free even for a little bit will be such a relief! I forgot what it means if it doesn't work (what does that indicate?). I wanted him to help me pin point what set off this multi-day pain fest, what did I do wrong. He said you probably didn't do anything wrong, this is just probably your new normal right now. I expressed how I felt lost and "unguided" without a physical therapist. He didn't think I needed one. He said I research things so well, he knows I'm not going to try anything like skiing, the ACL itself although still healing, it's generally not at risk for tearing (unless you do the same kind of move I did to tear it of course) so whatever I do I'm not really going to damage anything. Prior to this, I did contact a physical therapist who specializes in pain management therapy (90 miles away). No reply yet. I just always second guess what I should be doing. It would be nice to have someone to answer my PT questions! According to the US Women's Ski Team physical therapist who I've been writing to, he said physical therapy can be your friend when you have this bad graft pain. I'm doing it, but is it right? Right now it just feels like a guessing game. I'm trying to figure out what things I can do and not set me back on the couch for a week, rehab wise and general outdoor fun wise. Obviously it's not an easy or straight forward task! I've been reading about chronic pain integrated management, and just recently chronic pain and how yoga may build grey matter in the brain. Grey matter is brain tissue with numerous cell bodies and is located in the cerebral cortex and subcortical areas. Chronic pain is known to cause brain anatomy changes and impairments (this is now my excuse when I am forgetful or clumsy ha!) including less grey matter. Several studies indicate that when you practice yoga regularly you have more grey matter in the area of the brain that regulates pain. There are lots of articles out there on this. I have been doing yoga at home almost daily for about 3 months now. They said if you do it everyday it will change your life! I tried my third legit yoga class today, but it was a bit too much at this stage (class was called energizing flow). I finished the class though, but felt pretty swollen. I think I'll go back to the slow flow or restorative type yoga for a while longer. I'm almost 6 weeks into my "whole body/less ACL thinking/less worrying" experiment. This was at the suggestion of my physician assistant (assistant to my surgeon) to try for 6 weeks to see if we can lessen my knee pain. Good News: I successfully tried things that I haven't done in months which put a smile on my face (mountain biking, longest walk to date, walking in the snow, yoga classes, joined a gym). I am not pain free when I do these things, but I did them and was sore, but I could walk the next day. I do think I'm gaining some quad strength. Currently in week 14 of my "do over" rehab after I had a long hiatus of prescribed full rest. Bad News: The knee pain is still the same. Did I not do the experiment long enough? Do I try harder? Add more techniques? What was it supposed to accomplish? Was being pain free really the goal? Is it even possible to manage this kind of pain with the mind? I'm just bursting with questions! Overall, I use daily mantras of, "I am healing, I will heal, this isn't forever, I will get better, I have healed in the past." When I first tried it, it felt fake, I didn't believe it. Maybe now it doesn't feel as fake at least. I did not cure myself from random bouts of worrying, but I am going to continue this anyway. I do practice the "STOP! thinking" when I do start to worry, so I can divert my thoughts immediately. At least this wasn't a daily issue! Then after 5 weeks I just felt like something was really wrong, unsettling. I had to research more. This was all being too passive for my liking. I emailed professionals for advice. I've continued my research. I don't care if they say I'm hyper-focused on the knee, you and only you are your best advocate. I am getting hardly any physical therapy guidance, and am always questioning if I'm doing the right things. Below are two photos from my Thanksgiving desert camping trip (camping trip #13 of the year!) where I discovered I can ride a bike outside! I did four rides, two of which were legit mountain biking trails. One left me pretty sore. However, it felt so good to have wind on my face, legs spinning that I was smiling the entire time! Photo below: I walked in the SNOW as well! Almost a 4 mile hike on a road I've walked before, but now it's covered in snow. Snow is where I had my injury so it was a rather significant walk to me personally. I wore spikes on my shoes to prevent slipping and used poles. It felt like a workout and took me over 1.5 hours to walk it. Afterwards I felt like I had run a 10k! Photos below: My wall sits are progressing - I swore this was a 90 degree angle, but discovered not quite after I took a photo! I started with just 6 inches a couple months ago. Leg press machine at Planet Fitness - I won a Planet Fitness membership for 3 months. Great timing with winter here and all. At day 90 post op, I was doing 100 lbs with operative leg only! Now at day 300+ I am at 55 lbs with two legs, and thinking I need to drop it a bit more since I'm pretty sore in the tendon the next day. Just shows you how much work I still have to do. On to the research... I listened to podcasts on chronic pain treatments (Dr. Joe Tatta is a great resource). I've also contacted him on tendinopathy/tendonitis pain after surgical trauma. One of Dr. Tatta's podcast was with a tendon expert from Australia. I've also contact her with the same question asking how does surgical trauma tendinopathy vary from sports tendinopathy - aka do the same rules for isometric exercises and this top 10 things of what NOT to do (from Dr. Jill Cook) apply to my situation? For example, she says not to stretch the tendon, where as my surgical team (who has never seen my case) told me to stretch the tendon out more if it feels so tight. WHAT DOES A PERSON DO?!?!?!
I also contacted a sports psychologist after listening to another great podcast from The ACL Club. A phone call is scheduled this week to gather more info. Some days I just feel like I cannot do this alone anymore. I have many tools to use, but what if the tools aren't cutting it? Am I not doing them right and it's not working, or I am doing it right and this is the best it can do? I don't know!
I also contacted the US Women's Ski Team doctor. He has 20 years of female ACL/skier experience. I asked his team about tendonitis/tendinopathy this far out, what to do/not do, what to expect. His team wrote me back. His trainer said:
I also contacted another (third!) physical therapist. He is in the office where I went for the first 3 months of rehab. He suggested I do some isometric quad contractions everyday assuming this is tendinopathy, but we cannot be sure what it is. I wanted to know if a patient like me should really be left to her own devices doing rehab without guidance. He said typically he would meet a couple times with retests/revisits a month or so apart. My positive attitude: it is a work in progress. I have improved in lots of ways. Painful days are still tricky to remain positive. There you have it. I am researching again, I have burning questions, I have lots of information to process, new things to try (maybe not all at once). I just know being passive about my treatment was not working for me! |
AuthorA 45 year old active female who tore her ACL in January 2017 (at the age of 40). Reconstructive surgery in February 2017 with bone-patellar tendon-bone autograft. Archives
November 2022
|